Mumps Vaccination
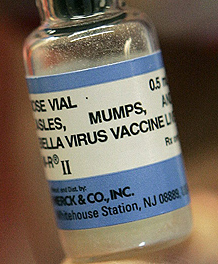 Overview
Overview
Mumps is one of several classic childhood diseases that ran rampant before the introduction of vaccination programs. The illness is caused by a virus transmitted by exhaled droplets from someone who is infected and lasts for anywhere from 7 to 10 days. Mumps is typically quite harmless and in a third of the cases does not even show any symptoms of illness.
The last third of its victims have painful swelling of the parotid and salivary glands (located in front of and below the ear and under the jaw). Infrequently, hearing loss will also occur with partial or complete recovery after the symptoms disappear.
Further complications can occur as inflammation of the pancreas. Complications are known to occur fairly frequently in adolescents and adults. There is also some risk that mumps can lead to encephalitis or meningitis, although neither typically becomes serious. In about 20 percent of the male adolescent and adults who become infected with mumps, inflammation of the testicles can also be a side effect. In rare cases, adolescent girls and women may come down with ovarian inflammation.
This illness gives a lifelong immunity to those who have it, even if no symptoms are present.
The Mumps Vaccine
Mumps vaccinations consist of attenuated live viruses which are injected into subcutaneous fatty tissue or muscle. Mumps vaccines are combined with inoculations against German measles (rubella) and measles in an MMR vaccine. Because live vaccines are involved, all combination and single vaccinations against mumps, measles and German measles are free of thiomersal.
Officials recommend infants receive their first vaccinations against mumps at about 13 months of age. Prior to this age, scientists believe antibodies received from the mother tend to cancel out the effect of a vaccination. The second vaccination should occur between the ages of three and five years old as a normal part of a pre-school program.
The vaccine can be given to adults who were not inoculated as children. The vaccination should not be given during pregnancy, and those women who have had an MMR vaccine should avoid becoming pregnant for at least one month after being vaccinated.
In European countries the aim is to eradicate this illness, as well as measles and German measles, but this would require a very high rate of vaccinations to take place. The overall vaccination rate in the UK has been too low to achieve this feat.
Vaccination Failures and Side Effects
Although efforts have been made to improve the vaccination, a few of those vaccinated do not develop (or develop too few) antibodies. In the long term the protective effect of vaccines based particularly on the Rubini strain (which is not available in the UK) has been deemed unsatisfactory. The recommended second vaccination does seem to improve the protective effect, although it is unclear if that protection last throughout one's life or is cut short. The Jeryl Lynn strain, which is currently in use in the UK, has shown up to 25 years of immunity against mumps.
Approximately one in 50 people who are vaccinated have a condition triggered called 'Vaccination mumps,' or in other words, are stricken with a weaker form of this illness. Symptoms include feeling generally unwell, accompanied by fever and a (usually) one-sided, painless swelling of the parotid gland. This usually takes place about three weeks after the vaccination.
In rare cases, a one-sided, painful swelling of the testicles can occur. A similar small risk for meningitis is triggered by the vaccine for mumps and is accompanied by headache, fever, stiff neck and vomiting. This condition does not become serious and leaves no lasting damage.
Recommendations and Considerations
Given the relatively small risk associated with mumps, as well as the possible usefulness for the child's development, a cautious approach would be to consider avoiding routine vaccinations for mumps.
Other researchers believe that mass vaccination leads to this illness being shifted to a later age (into adolescence and adulthood), when there is an increased risk for complications.
Further research is needed to confirm the persistence of lifelong immunity following vaccinations.
Caution is advised for children who have allergies to chicken proteins (eggs). However, this does not mean the vaccination should not be given: instead, a physician needs to be consulted before administering the vaccine. If the doctor decides the child has a real allergy to chicken protein the vaccine can be given under hospital supervision.
References
- Ada, G.L. (2000).Vaccination : the facts, the fears, the future. Sydney, N.S.W. : Allen & Unwin
- Godfrey, M. & Anderson, R. (2002). Exploding the myth of vaccination. Tauranga : R. Anderson
- Scheibner, V. (1993). Vaccination : 100 years of orthodox research shows that vaccines represent a medical assault on the immune system. Blackheath, NSW : V. Scheibner
- Studer, Hans-Peter. (2010). Vaccination : a guide for making personal choices. Edinburgh : Floris
Posted in Mumps Vaccination
Ask a Question Or Join a Discussion