Vaginitis
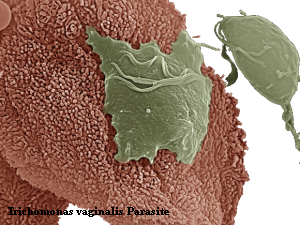 Overview
Overview
Vaginitis, an inflammation of the vagina, can occur as the result of several different factors, including bacterial or yeast infections, chlamydia, trichomoniasis, viral infections and low estrogen levels. The symptoms associated with this condition can include an itching or burning sensation in the vagina, vaginal discharge with a foul odor, abdominal discomfort, light vaginal bleeding and pain during intercourse or urination.
Causes of Vaginitis
Several different types of bacterial normally grow in the vagina. Called the normal flora, these bacteria help maintain a healthy environment in the vagina and aid in fighting off other organisms which may be more harmful. When on organism from the normal flora outgrows the others, bacterial vaginiosis occurs, disrupting the natural balance with the environment in the vagina. Women who have bacterial vaginosis frequently experience a greyish or white discharge that has an odor with a slightly "fishy" smell. The odor tends to be more prominent after the woman has sexual intercourse.
Yeast infections can be caused by fungi, the most common of which is Candida albicans. Vaginitis can occur as a result of yeast infections.
Women who suffer from diabetes have an increased risk of developing yeast infections.
Prevention
Some types of vaginitis can be prevented with the following guidelines:
- Good hygiene - Cleaning the genital area daily with a mild, fragrance-free and non-irritating soap helps this condition. Be sure to rinse the genital area and dry it well.
- Limit baths - Avoiding whirlpool spas and hot tubs is beneficial.
- Cotton underwear - Wearing under garments made of synthetic material or tights with synthetic crotches helps yeast to thrive in the vagina's moist environment. Wear cotton underwear and do not wear underwear to bed.
- Avoid scented objects - Do not use scented sanitary towels and tampons. The chemicals used to add fragrance to these particular products can irritate the vagina.
- Wiping the vagina - Wipe from front to back to avoid contaminating the vaginal area with more bacteria, especially after bowel movements.
- Never use douche - Douching is known to disrupt the normal flora of the vagina. This practice allows organisms to overgrow, which in turn causes infections to develop.
- Consume yogurt - Yogurt which contains active lactobacillus cultures may discourage or prevent the development of recurrent vaginal yeast infections.
- Practice safer sex - Use condoms to protect against STDs unless the relationship is monogamous and both partners have tested negative for infections.
Diagnosis
A health care professional can make an accurate diagnosis of vaginitis. This can be done by reviewing the patient's medical history and discussing symptoms and past vaginal infections or STDs. A pelvic examination allows the physician to check the genital area for lesions or discharge. A doctor may also choose to collect samples of vaginal discharges to have them analyzed to identify the cause of the vaginitis.
Treatments
Treatment processes will vary for vaginitis depending on the cause of the inflammation. Bacterial vaginitis can be treated with clindamycin or metronidazole, drugs which are commonly prescribed to treat infections. These two medications can be used in pill form or as vaginal gels and creams.
Antifungal drugs are also used to treat yeast infections. Suppositories and creams containing miconazole and clotrimazole are often given to women who are suffering from a vaginal yeast infection. These medications are available by prescription or as over-the-counter preparations. Oral antifungal medications, such as fluconazole, are also an option for treatment of vaginitis.
Metronidazole pills can be used to treat trichomoniasis. Antibiotics such as azithromycin, erythromycin, tetracycline or doxycycline are used to treat chlamydia.
No cure is currently available for herpes simplex virus and human papillomavirus. Physicians can prescribe antiviral medications such as famciclovir, valacyclovir and acyclovir to minimize outbreaks and discomfort.
For removing genital warts, surgery or topical medications can be used.
Natural Treatments
Eating a balanced and healthy diet can aid in keeping the body's acid-alkaline balance where it should be. Avoid fruit yogurts and probiotic drinks, which contain too much sugar (almost anything containing sugar encourages unhealthy bacteria to flourish). Avoid alcohol while the infection is running its course as well. Vegetables which are rich in beta-carotene are good choices, as the body will use the vitamin A to help boost the body's immunity. Yellow, orange and red fruits and vegetables are good sources.
Supplements
Several supplements can help to strengthen the body's internal structure, helping to prevent the spread of infection. They include:
- B-Complex vitamins - Vitamin B helps the body form healthy cells to replace cells which are infected.
- Vitamin C - The bioflavonoids help boost immunity and strengthen body structures.
- Vitamin E - Open a vitamin E capsule and gently rub the oil around the vagina.
- Zinc - This immunity booster helps the body to heal faster.
- Probiotics - The vagina can recolonize its good bacteria if the woman consumes more probiotics. Capsule forms are available. For a double effect, take an oral probiotic and use a vaginal pessary containing beneficial bacteria.
Herbs
Some herbs are especially helpful for healing vaginitis. They include:
- Barberry root bark - This herb contains an alkaloid called berberine, which is known to be effective against fungal and bacterial infections.
- Echinacea - This herbal remedy has a strong antimicrobial effect to help in fighting off infections.
- Garlic - This herb is highly effective for optimal health and has well-known antibacterial properties. Garlic supplements will give the body's immune system a boost.
- Marigold - This healing herb is also antimicrobial.
References
- Bratman, S. The Alternative Medicine Ratings Guide: an expert panel rates the best treatments for over 80 conditions, Prima Health A Division of Prima Publishing (1998)
- Brown, L. Alternative Medicine, NTC/Contemporary Publishing (1999)
- Canas, M. et al. (2006). Women's health. Barcelona, Spain : Rebo
- Glenville, M. (2010).The natural health bible for women : the complete guide for women of all ages.London : Duncan Baird Publishers
- Deepak Chopra, M.D. Alternative Medicine: The Definitive Guide, Celestial Arts (2002)
- Jarvis, S.(2009).Women's health for life : medical advice you can trust : symptoms, treatment, prevention. London : Dorling Kindersley
- Servan-Schreiber, D. The Encyclopedia of New Medicine: Conventional & Alternative Medicine For All Ages, Rodale International Limited (2006)
Posted in Vaginitis
Ask a Question Or Join a Discussion